It would have been way easier than it currently is for women to get an early endometriosis diagnosis, if not for several factors. Chief among these factors is the fact that there are no peculiar symptoms for endometriosis.
Even worse, no simple sample or swab can be taken and tested to give a correct diagnosis of endometriosis. Its symptoms are often mistaken for menstrual pain, and at later stages, UTI, hormonal imbalance and other conditions. Our wellness guide focuses on holistic women’s health, but we spotlight endometriosis in this article because it is a real concern for women.
What Is Endometriosis?
According to the World Health Organisation, endometriosis is a health condition where tissue similar to the lining of the womb grows elsewhere in the body, and this causes inflammation and scar tissue formation. This intruding tissue can grow in a number of places outside the uterus, such as the ovaries, pelvic lining, the fallopian tubes, bowel and bladder.
Sources from mayoclinic show that it can even appear in unlikely areas such as the diaphragm, lungs, or surgical scars. This tissue typically behaves like uterine lining, mimicking everything it would do. It responds to hormones, thickens, breaks down, and bleeds during the menstrual cycle. However, because it has no way to exit the body, it triggers the inflammation and scar tissue formation we mentioned earlier, and often, it comes with other complications such as adhesions, and severe endometriosis symptoms such as chronic pain.
How Long Does It Take to Get Diagnosed With Endometriosis?
Endometriosis is not recognised for what it is at first check-in very often, which is why many women experience a long wait before receiving a confirmed diagnosis. This is because the symptoms vary widely, and are interchangeable with symptoms of stress-related ailments, and even other reproductive conditions such as, severe menstrual pain, chronic pelvic pain, painful intercourse, fatigue, irritable bowel syndrome and even urinary tract infections.
Currently, laparoscopy is the most accurate method to diagnose endometriosis, but it is an invasive surgical procedure that requires anesthesia and specialized surgical expertise. Many healthcare professionals lack the expertise required to carry out this procedure safely.
In addition, laparoscopy is not recommended as a first method to employ for diagnosis for every patient because of the inherent risks, including surgical complications, recovery time, and the cost of the procedure. This is typically what causes delay in endometriosis diagnosis.
An alarming 10% of women of reproductive age are affected by endometriosis, says WHO, and because of this statistic, it might have been puzzling if it wasn’t the reality that diagnosis is rarely immediate. Multiple studies show that the average timespan for delay in endometriosis diagnosis is about 7 years from the onset of symptoms, while other sources say 4-12 years is the benchmark. This delay has some serious consequences, including:
- Progression of disease
- Chronic pelvic pain
- Reduced quality of life
- Mental health strain
- Fertility issues
- Expensive healthcare costs
What Causes Endometriosis?
There is no single confirmed cause of endometriosis. Medical evidence shows that it develops due to a combination of genetic, hormonal, immune, and environmental factors, and we will discuss them below:
Genetic Susceptibility
Endometriosis is polygenic, meaning multiple genes contribute to risk rather than one inherited mutation. Research shows higher incidence among people with first-degree relatives (mother, sister, aunt) who have the condition, indicating a strong hereditary component related to immune regulation and hormone sensitivity.
Retrograde Menstruation
Retrograde menstruation occurs when menstrual blood flows backward through the fallopian tubes into the pelvic cavity. This theory, proposed in the 1920s, suggests that endometrial cells implant outside the uterus and begin to grow. However, because most menstruating women experience some retrograde flow without developing endometriosis, this theory alone does not fully explain the disease.
Hormonal Imbalance
Hormonal imbalance is a key factor to consider here because estrogen plays a central role in endometriosis development and progression. Excessive estrogen levels in a woman’s body or heightened tissue sensitivity promote lesion growth and inflammation. Many patients also show signs of progesterone resistance, which reduces the body’s ability to regulate abnormal tissue growth. It would seem that because of this alone, women should take balancing their hormones more seriously, both through medical procedure and certified natural means.
Immune System Dysfunction
In a healthy immune system, misplaced endometrial cells are destroyed. In endometriosis, immune dysfunction allows these cells to survive, implant, and proliferate, contributing to chronic inflammation.
Environmental Exposure
Endocrine-disrupting chemicals such as dioxins, phthalates, and BPA can interfere with hormone balance and immune responses. While not direct causes, they may increase susceptibility in genetically predisposed individuals.
Surgical Transplantation
In rare cases, endometrial tissue can be transferred during surgeries such as cesarean sections or hysterectomies, leading to endometriosis growth in surgical scars.
Why Is Endometriosis Hard to Diagnose?

Source: Pinterest
Several factors contribute to prolonged endometriosis diagnosis. There has been a lot of inquiry into the foundational reasons why endometriosis is so hard to diagnose, and here are some research findings:
Under-recognition Within Primary Care Setting
Many primary care providers receive limited training on recognizing early or atypical endometriosis symptoms. As a result, pelvic pain is often attributed to stress, infections, or “normal” menstruation, delaying referral to specialists.
Painful periods are common quite alright, but endometriosis pain is typically more severe, persistent, and disruptive. When this distinction is not recognized, the opportunity to diagnose early goes by and the patient would then have to suffer more needless pain in the future.
Symptom Variability

Source: Pinterest
Endometriosis symptoms does not present the same way in everyone. Symptom severity does not always correlate with disease extent, making recognition more complex.
Common Endometriosis Symptoms
- Chronic pelvic pain
- Severe menstrual cramps (dysmenorrhea)
- Heavy or prolonged menstrual bleeding
- Pain during or after penetrative sex
- Painful bowel movements
- Painful or frequent urination
- Gastrointestinal symptoms (bloating, constipation, diarrhea)
- Fatigue
- Lower back pain
- Infertility
Because these symptoms overlap with other conditions, diagnosis is frequently delayed.
Gender Bias In Pain Assessment

Source: Unsplash
The pain women suffer has historically been underestimated in medical settings. It’s almost as though women are expected to endure whatever pains they experience as part of their womanly lot in life. Pelvic pain is often seen as a normal part of womanhood, leading to dismissal even when these symptoms interfere with daily life, education, employment and relationships.
No doubt, this bias has caused an underestimation in the medical care allotted to women who may have endometriosis and an often costly delay in referring cases to healthcare specialists.
Diagnostic Limitations
There is currently no reliable blood test or biomarker for early endometriosis detection. Imaging tools such as ultrasound and MRI may identify ovarian endometriosis or the disease in advanced stages but frequently miss those superficial lesions that can aid early diagnosis.The gold standard for diagnosis remains laparoscopy, a minimally invasive surgical procedure that allows direct visualization and biopsy. However, surgery is often delayed due to cost, limited access to skilled surgeons, and reluctance to recommend invasive procedures early.
Socioeconomic Barriers
Diagnosis often requires multiple specialist visits, advanced imaging, and sometimes surgery. In healthcare systems with high out-of-pocket costs, individuals with limited financial resources experience significantly longer delays.
Insufficient Public Awareness
Many people are unaware of what constitutes abnormal menstrual pain. Cultural silence around menstruation and pelvic health discourages open discussion about it, leading many to tolerate symptoms for years before seeking help. For many women, pains like this are a part of reality, and they’d usually ignore it until it is no longer possible to do so, or it causes a complication.
Patient Advocacy: What to Do While You’re Waiting for a Diagnosis
If you suspect that you may have endometriosis, and not just menstrual cramps and feel stuck in the diagnostic waiting phase, self-advocacy could save you more pain, heavier medical bills and complications from being a prolonged carrier with treatment. Preparing targeted questions can help move the process forward. Patient advocacy refers to supporting and empowering women who may be suffering from endometriosis to navigate the healthcare system, understand their symptoms, and actively participate in decisions concerning their diagnosis and treatment.
Because doctors often underdiagnose endometriosis and misinterpret or dismiss its symptoms. Patient advocacy ensures that healthcare providers hear concerns, investigate them properly, and take appropriate action. This is why we have curated these questions to enable you to interact with your health officers in a way that leaves you informed about your particular case, and sets you on the path to a confirmed endometriosis diagnosis.
Three Questions to Ask Your Doctor
- “Based on my symptoms, could this be endometriosis, and what steps can we take to rule it in or out?”
This encourages your provider to formally consider endometriosis rather than dismiss symptoms. - “Can I be referred to a gynecologist or endometriosis specialist for further evaluation?”
Early referral improves diagnostic accuracy. - “What diagnostic options are appropriate at this stage, and what are the risks and benefits of each?”
This opens discussion about imaging, medical management, and potential laparoscopy.
Make sure that you track your symptoms, as this will definitely help your case more.
Can Endometriosis Be Prevented?
Source: Unsplash
While doctors cannot completely prevent endometriosis, certain strategies may reduce the risk or slow its progression.
- Maintaining healthy estrogen levels through regular exercise and limiting alcohol
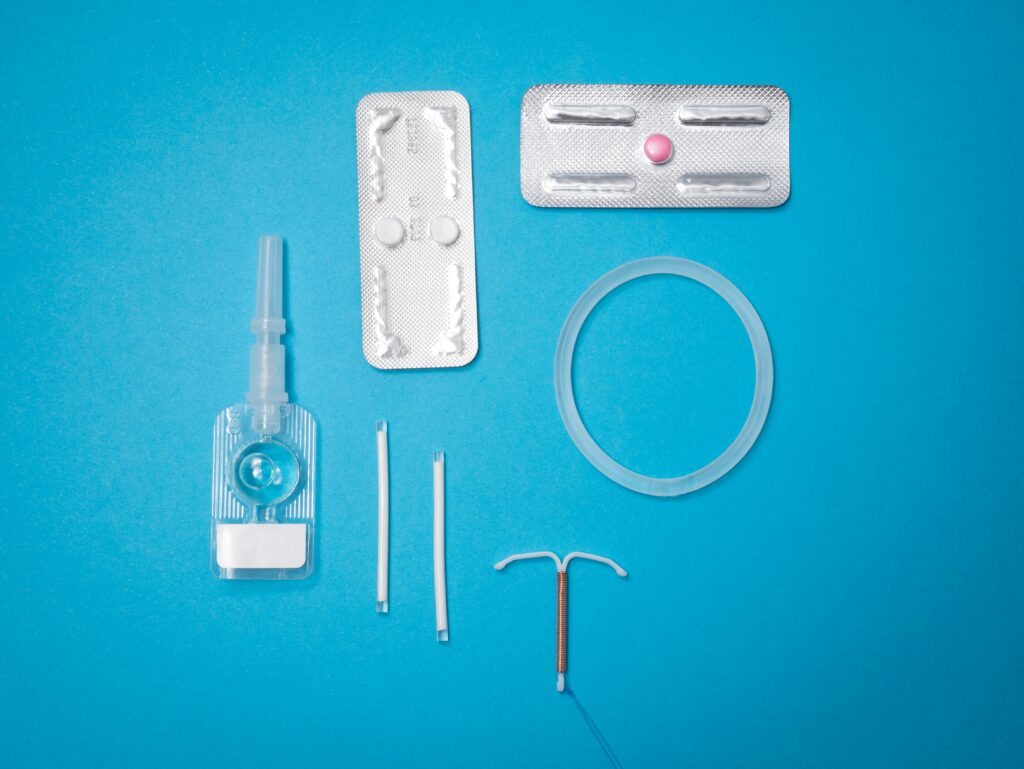
- Using hormonal treatments such as oral contraceptives or hormonal IUDs to suppress ovulation
- Following anti-inflammatory dietary patterns rich in fruits, vegetables, whole grains, and omega-3 fatty acids
- Reducing exposure to endocrine-disrupting chemicals
- Avoiding unnecessary pelvic surgeries when possible
- Knowing family medical history to support early evaluation
To wrap up, gaps in medical care, medical bias, and limited diagnostic tools create a systemic challenge. This leads to the long wait for an endometriosis diagnosis. This article has carefully addressed how one can bypass these challenges. And get an early diagnosis, so that treatment can commence sooner.



